Outcomes of robotic living donor right hepatectomy from 52 consecutive cases: Comparison with open and laparoscopy-assisted donor hepatectomy
Seoung Yoon Rho1, Jae Geun Lee1, Dong Jin Joo1, Myung Soo Kim1, Soon Il kim1, Dai Hoon Han1, Jin Sub Choi1, Gi Hong Choi1.
1Surgery, Yonsei University College of Medicine, Seoul, Korea
Objective: To investigate the feasibility and safety of an alternative robotic living-donor right hepatectomy (RLDRH) technique.
Summary Background Data: Data for minimally invasive living-donor right hepatectomy, especially RLDRH, in a relatively large donor cohort have not been reported yet.
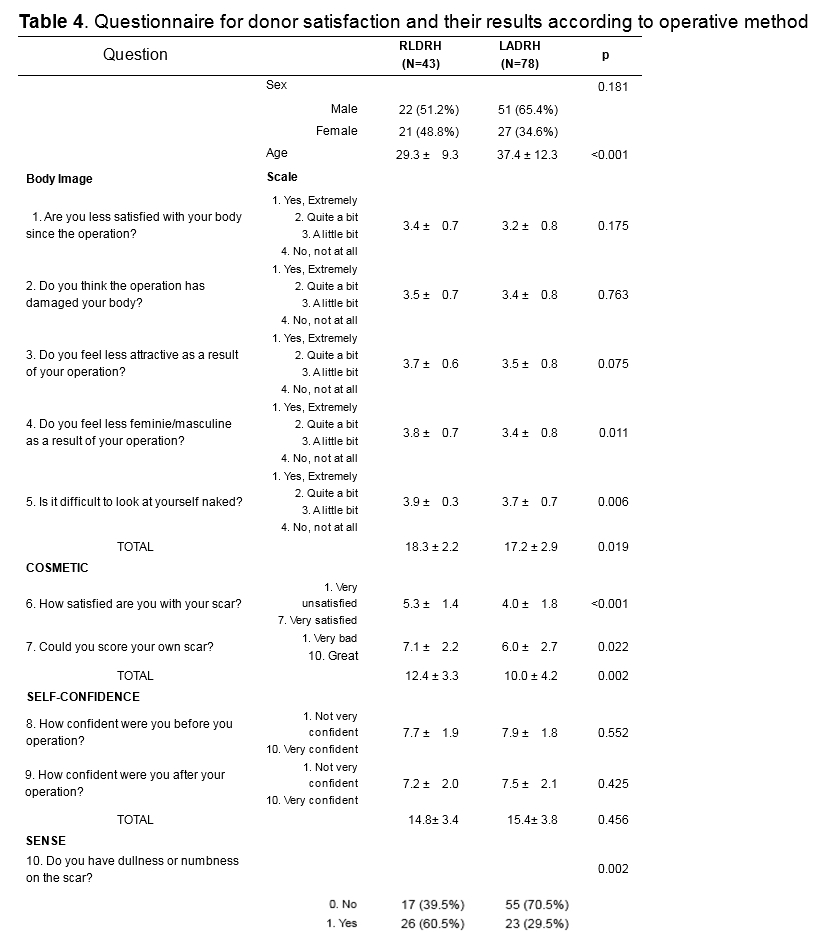
Methods: From March 2016 to March 2019, 52 liver donors underwent RLDRH. The clinical and perioperative outcomes of RLDRH were compared with those of conventional open donor right hepatectomy (CODRH; n=62) and laparoscopy-assisted donor right hepatectomy (LADRH; n=118). Donor satisfaction with cosmetic results was compared between RLDRH and LADRH using a body image questionnaire.
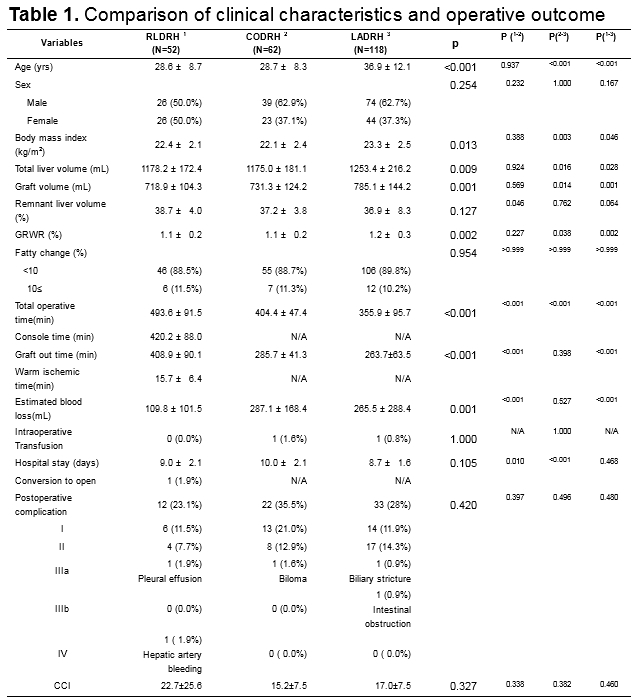
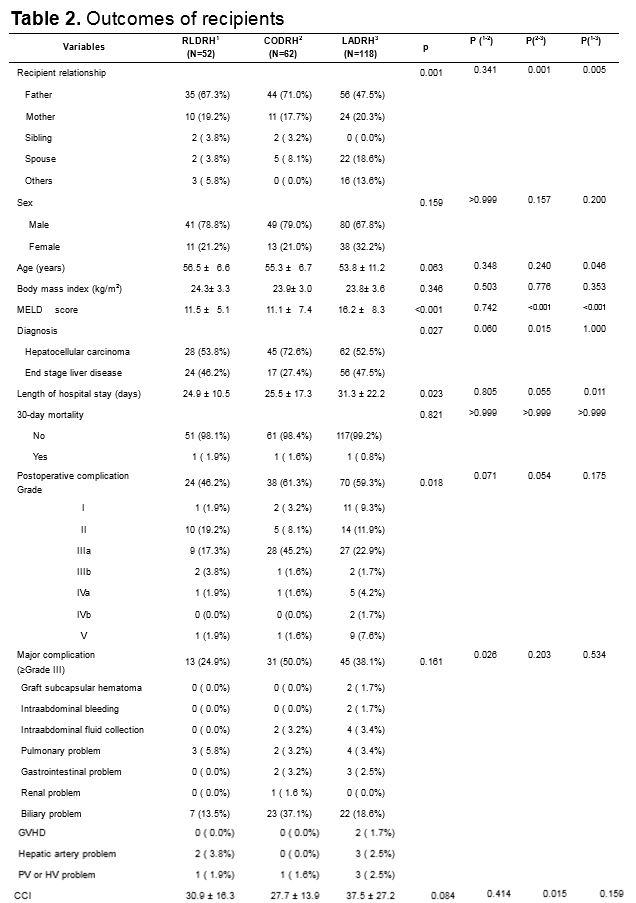
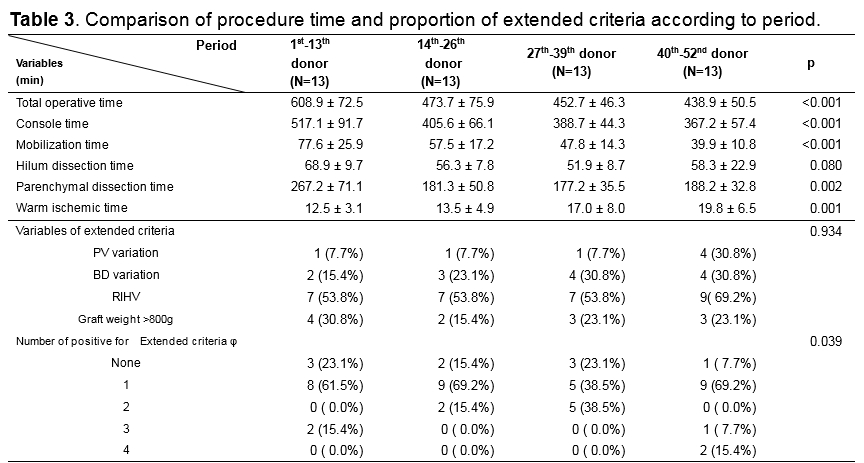
Results: Although RLDRH had a longer operative time (RLDRH, 493.6 min; CODRH, 404.4 min; LADRH, 355.9 min, p<0.001), its mean estimated blood loss was significantly lower (RLDRH, 109.8 mL; CODRH, 287.1 mL; LADRH, 265.5 mL; p=0.001). The postoperative complication rates were similar among the three groups (RLDRH, 23.1%; CODRH, 35.5%; LADRH, 28.0%; p=0.420). Regarding donor satisfaction, the body image and cosmetic appearance scores were significantly higher in RLDRH than in LADRH. There was no significant difference in hospital stay among the three groups (p=0.105). After propensity score matching, RLDRH showed a shorter hospital stay and similar complication rate comparing CODRH.
Conclusions: RLDRH resulted in a similar postoperative complication rate and shorter length of hospital stay compared with those of CODRH and provided better body image and cosmetic results compared with those of LADRH. RLDRH is feasible and can be safely performed by expert surgeons in both robotic systems and open hepatectomy.
[1] Adam R, Karam V, Delvart V, et al. Evolution of indications and results of liver transplantation in Europe. A report from the European Liver Transplant Registry (ELTR). J Hepatol. 2012;57:675-688.
[2] Chen C-L, Kabiling CS, Concejero AM. Why does living donor liver transplantation flourish in Asia? Nature Reviews Gastroenterology &Amp; Hepatology. 2013;10:746.
[3] Barr ML, Belghiti J, Villamil FG, et al. A report of the Vancouver Forum on the care of the live organ donor: lung, liver, pancreas, and intestine data and medical guidelines. Transplantation. 2006;81:1373-1385.
[4] Ratner LE, Sandoval PR. When disaster strikes: death of a living organ donor. Am J Transplant. 2010;10:2577-2581.
[5] Cheah YL, Simpson MA, Pomposelli JJ, et al. Incidence of death and potentially life-threatening near-miss events in living donor hepatic lobectomy: a world-wide survey. Liver Transpl. 2013;19:499-506.
[6] Rossler F, Sapisochin G, Song G, et al. Defining Benchmarks for Major Liver Surgery: A multicenter Analysis of 5202 Living Liver Donors. Ann Surg. 2016;264:492-500.
[7] Shirabe K, Eguchi S, Okajima H, et al. Current Status of Surgical Incisions Used in Donors During Living Related Liver Transplantation-A Nationwide Survey in Japan. Transplantation. 2018;102:1293-1299.
[8] Wang SH, Lin PY, Wang JY, et al. Mental health status after living donor hepatectomy. Medicine (Baltimore). 2017;96:e6910
[9] Ciria R, Cherqui D, Geller DA, et al. Comparative Short-term Benefits of Laparoscopic Liver Resection: 9000 Cases and Climbing. Ann Surg. 2016;263:761-777.
[10] Koffron AJ, Kung R, Baker T, et al. Laparoscopic-assisted right lobe donor hepatectomy. Am J Transplant. 2006;6:2522-2525.
[11] Suh KS, Hong SK, Lee KW, et al. Pure laparoscopic living donor hepatectomy: Focus on 55 donors undergoing right hepatectomy. Am J Transplant. 2018;18:434-443.