Ambient air pollution and waitlist mortality among lung transplant candidates
Yijing Feng1, Miranda Jones1, Nadia Chu1, Dorry L. Segev1, Mara McAdams DeMarco1.
1Johns Hopkins, Baltimore, MD, United States
Introduction: Previous studies suggested that air pollution is associate with higher risk of respiratory diseases and accelerated decline in lung function among general population. However, few studies have examined the effect of fine particulate matter (particles <2.5μm in diameter [PM2.5]) among the population with advanced stage pulmonary diseases. Here we seek to investigate the association between PM2.5 and waitlist mortality among lung transplant candidates in the United States (US).
Materials and Methods: Lung transplant candidates listed in the US between January 1st 2010 and December 31st 2016 were identified from Scientific Registry of Transplant Recipients. PM2.5 concentrations for 2010-2016 were obtained from NASA’s SEDAC Global Annual PM2.5 Grids. Annual PM2.5 concentration at the year of listing was estimated at each participant’s zip code. We estimated multivariable adjusted hazard ratios (95% confidence intervals [CI]) for waitlist mortality using Cox proportional hazards regression.
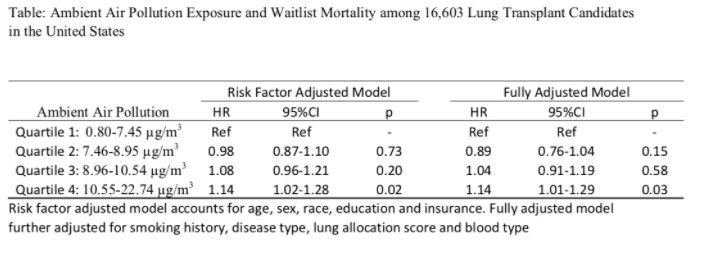
Results and Discussion: Among 16,603 candidates with PM2.5 exposure, mean age at listing was 56, 43.8% were female and 81.7% were non-Hispanic white. The ZIP Code level PM2.5 concentration ranged from 0.80-7.45, 7.46-8.95, 8.96-10.54, 10.55-22.74 µg/m3 respectively in quartiles 1 through 4. When compared to those who were living in the zip code with lowest quartile of PM2.5 exposure, candidates living in zip codes in the highest quartile of PM2.5 exposure had 1.14 (95%CI 1.02-1.28) times higher hazard of waitlist mortality after adjusted for demographics and SES (Table). The result remained significant after further adjusted for smoking, disease type, lung allocation score and blood type (HR=1.14; 95%CI 1.01-1.29).
Conclusion: Among US lung transplant candidates, exposure to PM2.5 above 10.55 µg/m3 was associated with increased risk for waitlist mortality. Importantly, this threshold for exposure to ambient air pollution is well below the US Environmental Protection Agency’s National Ambien Quality Standard for PM2.5 of 12 µg/m3 suggesting that lung transplant candidates may be at risk even in regions with relatively lower air pollution. These findings highlight the importance of considering the contribution of environmental exposures, such as ambient air pollution to long-term outcomes of lung transplant candidates.