Continuous peri-operative regional analgesia by asymmetrical Erector Spinae Plane Blocks on live liver donors for liver resection: A cases serie retrospective analysis
Philippe Macaire1, Viet Vu1, Chinh Quach1, Vicente Rocques2, Chi Nguyen3.
1Anesthesiology and Pain, VinMec International Hospital , Hanoi, Viet Nam; 2Anesthesiology and Critical Care Medicine, Hospital Virgen de la Arrixaca, , Murcia, Spain; 3Research and Biostatistics, VinMec Healthcare System, Hanoi, Viet Nam
Introduction: Open surgical resection for living liver donation may cause severe postoperative pain and promote a high risk of pain chronicisation if not treated adequately 1-7. This may have a significant effect on the patient's every day quality of life 8,9.
All multimodal analgesia regimen including paracetamol, nefopam, nonsteroidal anti-inflammatory drugs, gabapentin, steroids and opioids has not been demonstrated to be optimal 10,11. To date implementation of regional analgesia seems to be a better choice 12-17. However, the use of thoracic epidural anesthesia raise some concerns related to their potential complications 18. The erector spinae plane block (ESPB) is an interfascial plane block whereby local anesthetic is injected within a plane beneath the iliocostalis, longissimus, and spinalis muscles to achieve multi-metameric analgesia for thoracic or abdominal surgeries 19.
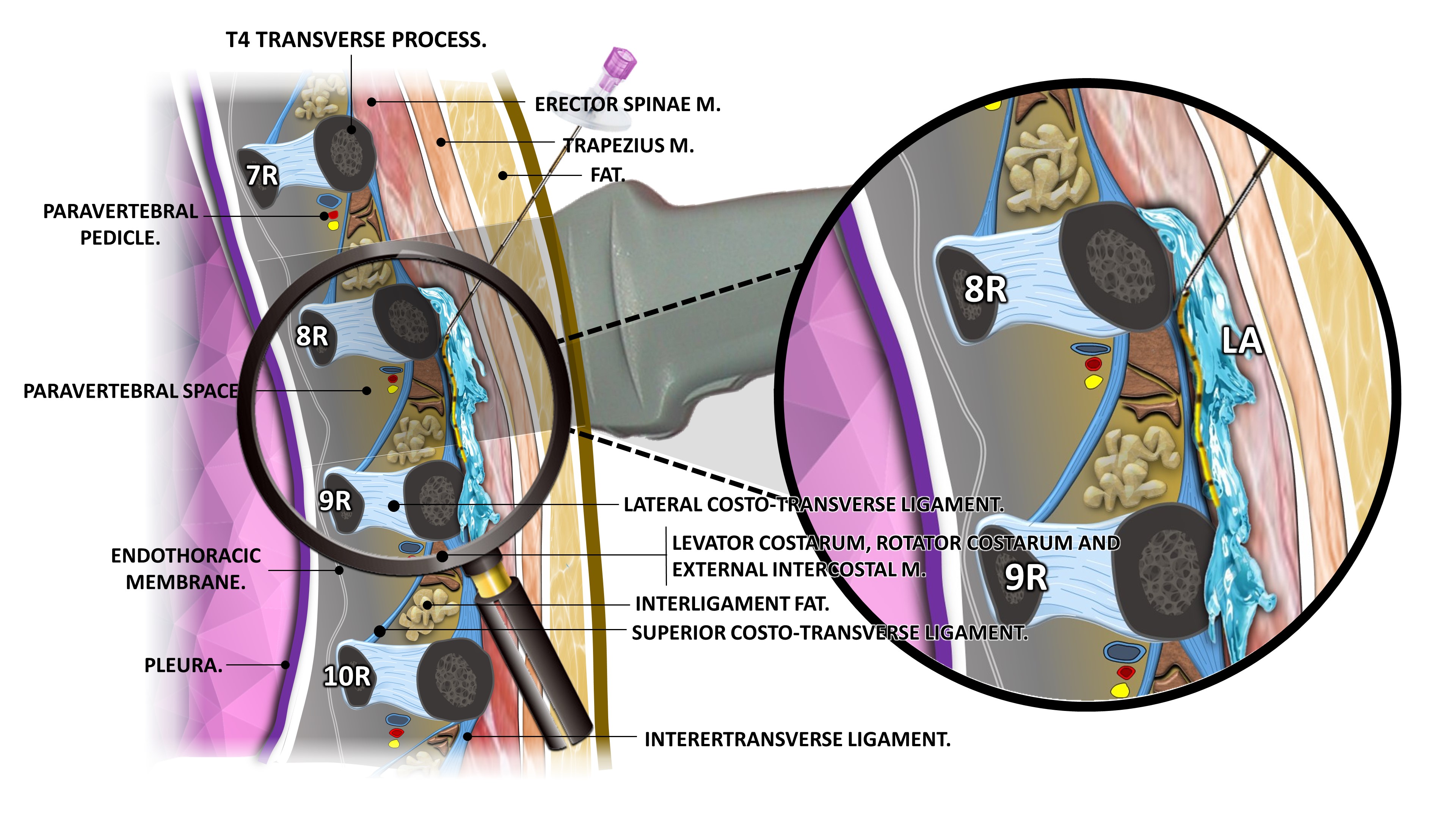
Its effect appears to be due to local anesthetic spread close to/into the paravertebral space, affecting both the dorsal and ventral rami of the thoracic spinal nerves. The Authors reported recently that a bilateral continuous shot ESPB provided an efficient and safe pain relief opioid free after open cardiac surgery compared with systemic analgesia 20.
The authors of the present study hypothesized that live liver donors undergoing open liver resection using continuous ESPB and opioid-sparing analgesia would be more likely to have an efficient coverage of the pain territories with low VAS scores in post operative without any complication. The originality was to provide asymmetrical targeted analgesia from T5 to T8 on the left side and T5 to T11 on the right side.
Material and Methods: Ethical approval 75/2020/QĐ-VMEC we analyzed 16 live liver donors adult patients for elective liver resection surgery. After usual Anesthesia induction for these surgeries, the bilateral insertion of ESP catheter was performed under Ultrasound (US) guidance at T6 level on left side and T8 level on right side by anesthesiologist recently trained to the technique. After US verification of the position of the tip catheter in the interfacial plane at T7 (left) and T9 (right) an induction dose of Ropivacaine (ROP) 0.5% 0.25mL/kg/Right side 0.10mL/kg/left side was given 30 minutes before incision.
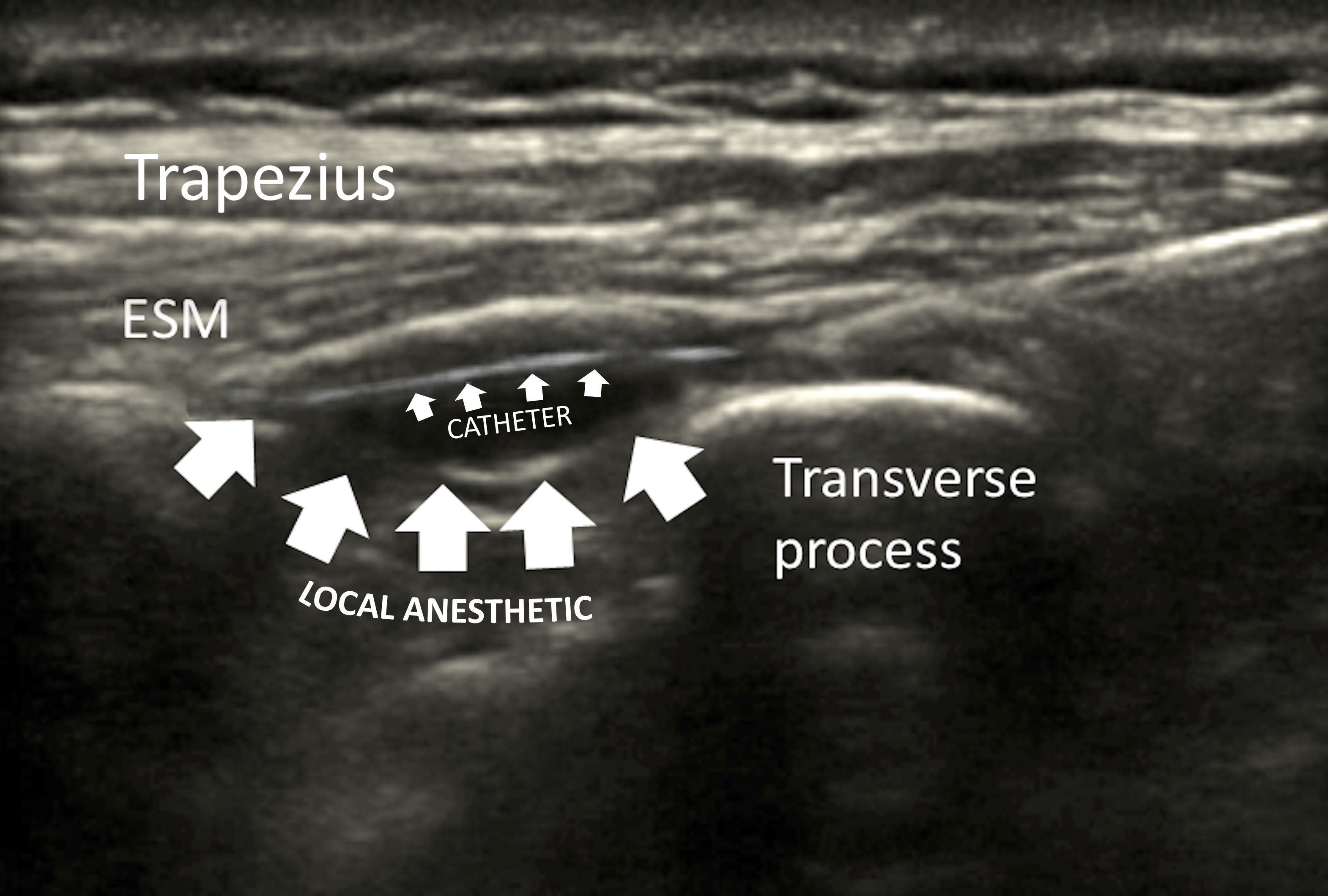
At the end of the surgery an infusion of Prorammed Intermittent Bolus (PIB) of ROP 0.2% (0.20mL/kg/Right side - 0.10mL/kg/left side) /6h was started with opioid rescue for 3 days. The volume of was adapted to extension of block after extubation.
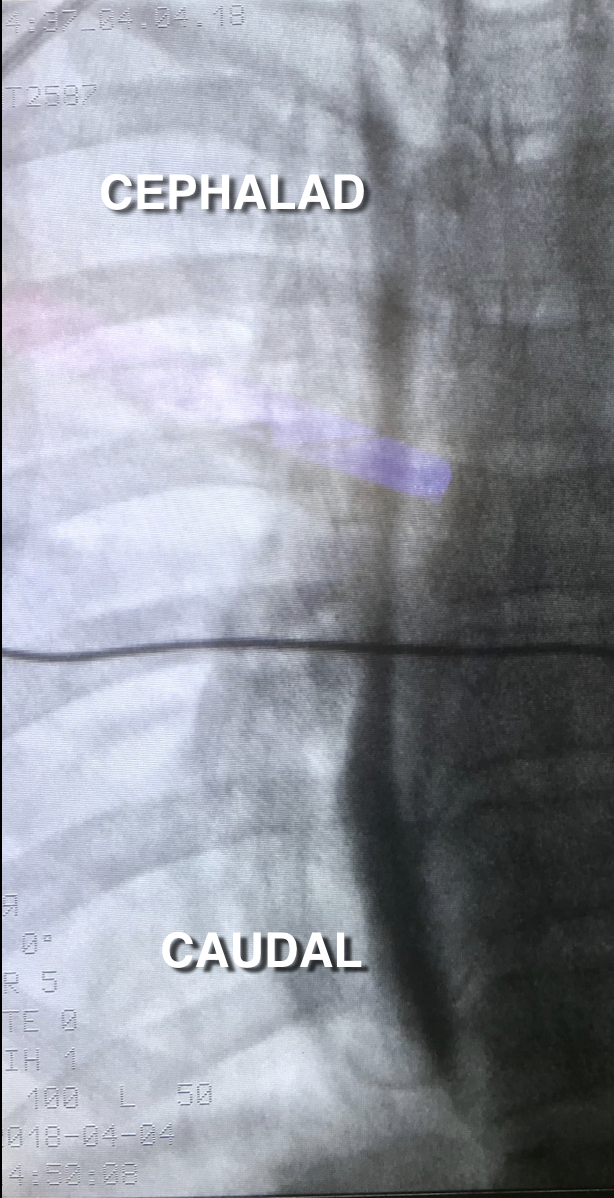
Results: Average VAS at rest at any time point < 2, average VAS at mob at any time point <3.125. Only 9 patients replied for follow up. At 1 month and 6 month: 77.78% (7/9 patients) has no pain, only 1 patient has pain (VAS=5). At 12 month: 66.67% (6/9 patients) has no pain, 3/9 patients has pain VAS-score=5.
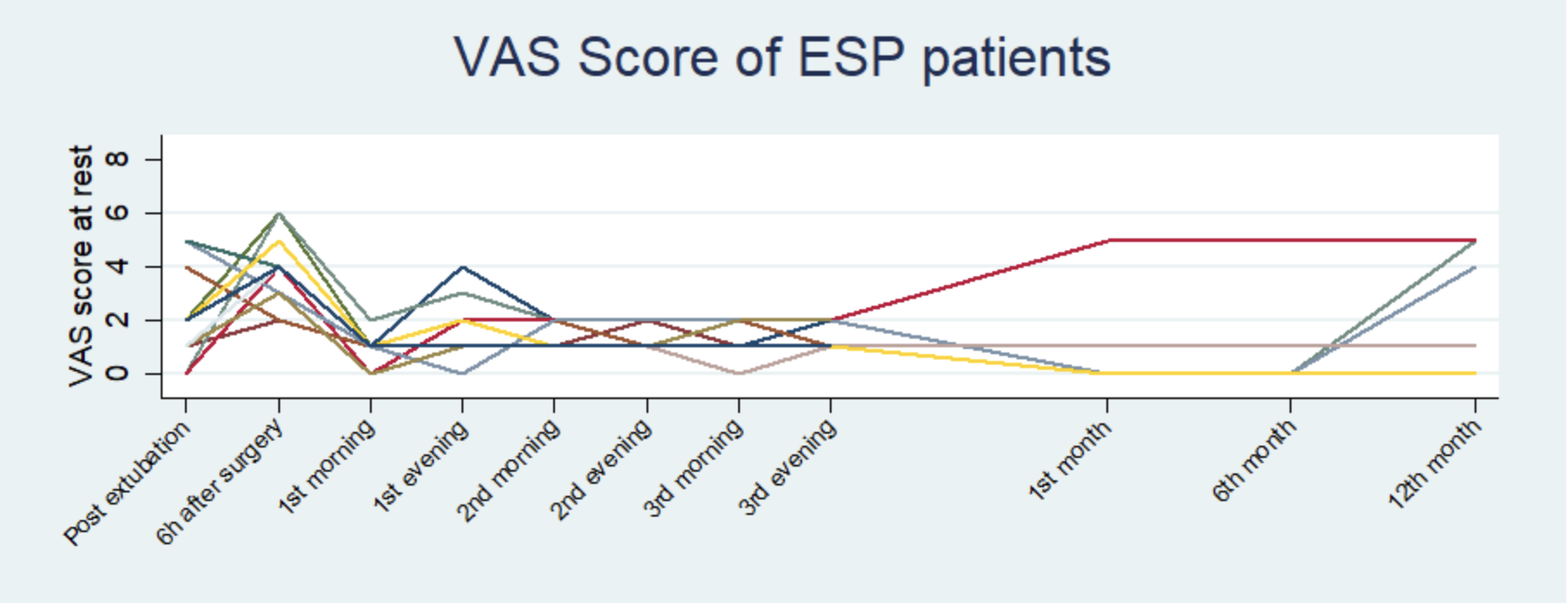
For 8/16 patients volume of PIB was increased by 0.05 mL/kg-h. Only 2 patients using rescue morphine for 3 days. No incident or hematomae. all block fully recovered after ESP catheter.
Discussion: Clinical results indicate that local anesthetic injected over the transverse process and beneath the erector spinae muscle spreads cranial and caudal to achieve multiple vertebral levels, and reaches the paravertebral space to anesthetize dorsal and ventral ramus as well as the rami communicants which supply the sympathetic chain. Doses of local anesthetics are very low due to the PIB (144-168 mg of Ropivacaine/day for a 60kg patient).
Conclusion: For the first time, this cases serie showed that continuous peri-operative analgesia by ESP blocks is effective & safe for live liver donnor. It needs more studies to evaluate all benefits on the surgical outcomes.
[1] Holtzman S, Clarke HA, McCluskey SA, Turcotte K, Grant D, Katz J. Acute and chronic postsurgical pain after living liver donation: Incidence and predictors. Liver Transpl. 2014 Nov;20(11):1336-46
[2] Soyama A, Takatsuki M, Hidaka M, Imamura H, Kuroki T, Eguchi S. Acute and chronic postsurgical pain after living liver donation: Incidence and predictors. Liver Transpl. 2015 Aug;21(8):1109.
[3] Kehlet H, Jensen TS, Woolf CJ. Persistent postsurgical pain: risk factors and prevention. Lancet. 2006 May 13;367(9522):1618-25.
[4] Martinez V, Baudic S, Fletcher D. Chronic postsurgical pain. Ann Fr Anesth Reanim. 2013 Jun;32(6):422-35.
[5] D. Fletcher, V. Martinez, Opioid-induced hyperalgesia in patients after surgery: A systematic review and a meta-analysis, Br J Anaesth 112 (2014)991–1004.
[6] F.M. Perkins, H. Kehlet, Chronic pain as an outcome of surgery, Anesthesiology 93 (2000) 1123–1133.
[7] D. Fletcher, U.M. Stamer, E. Pogatzki-Zahn, (euCPSP group for the Clinical Trial Network group of the European Society of Anaesthesiology), Chronic postsurgical pain in Europe: An observational study, Eur J Anaesthesiol 32 (2015) 725–734.
[8] Chan SC, Liu CL, Lo CM, Lam BK, Lee EW, Fan ST. Donor quality of life before and after adult-to-adult right liver live donor liver transplantation. Liver Transpl. 2006 Oct;12(10):1529-36
[9] Parsons B, Schaefer C, Mann R, Sadosky A, Daniel S, Nalamachu S, et al. Economic and humanistic burdenof post-trauma and post-surgical neuropathic pain among adults in the United States. J Pain Res 2013;17:459-469.
[10] Lee SH, Lim KC, Jeon MK, Kim IO, Jeong JS, Hong JJ, Ha HS. Postoperative pain and influencing factors among living liver donors. Transplant Proc. 2012 Mar;44(2):363-5.
[11] Kao CW, Wu SC, Lin KC, Chen CL, Huang CJ, Cheng KW, Jawan B, Wang CH. Pain management of living liver donors with morphine with or without ketorolac. Transplant Proc. 2012 Mar;44(2):360-2
[12] F. Carli, H. Kehlet, G. Baldini, et al., Evidence basis for regional anesthesia in multidisciplinary fast-track surgical care pathways, Reg Anesth Pain Med 36 (2011) 63–72.
[13] M.H. Andreae, D.A. Andreae, Regional anaesthesia to prevent chronic pain after surgery: A Cochrane systematic review and meta-analysis, Br J Anaesth111 (2013) 711–720.
[14] Levene JL, Weinstein EJ, Cohen MS, Andreae DA, Chao JY, Johnson M, Hall CB, Andreae MH. Local anesthetics and regional anesthesia versus conventional analgesia for preventing persistent postoperative pain in adults and children: A Cochrane systematic review and meta-analysis update. J Clin Anesth. 2019 Aug;55:116-127.
[15] Clarke H, Chandy T, Srinivas C, Ladak S, Okubo N, Mitsakakis N, Holtzman S, Grant D, McCluskey SA, Katz J. Epidural analgesia provides better pain management after live liver donation: a retrospective study. Liver Transpl. 2011 Mar;17(3):315-23.
[16] Richebé P, Capdevila X, Rivat C. Persistent Postsurgical Pain: Pathophysiology and Preventative Pharmacologic Considerations. Anesthesiology. 2018 Sep;129(3):590-607.
[17] Bonnet A, Lavand'homme P, France MN, Reding R, De Kock M. Postoperative pain trajectories to identify risk of chronic postsurgical pain in living donors for liver transplantation. Ann Fr Anesth Reanim. 2012 Dec;31(12):945-9.
[18] H. Freise, H.K. Van Aken, Risks and benefits of thoracic epidural anaesthesia, Br J Anaesth 107 (2011) 859–868.
[19] M. Forero, S.D. Adhikary, H. Lopez, et al., The erector spinae plane block, Reg Anesth Pain Med 41 (2016) 621–627.
[20] Macaire P, Ho N, Nguyen T, Nguyen B, Vu V, Quach C, Roques V, Capdevila X. Ultrasound-Guided Continuous Thoracic Erector Spinae Plane Block Within an Enhanced Recovery Program Is Associated with Decreased Opioid Consumption and Improved Patient Postoperative Rehabilitation After Open Cardiac Surgery-A Patient-Matched, Controlled Before-and-After Study. J Cardiothorac Vasc Anesth. 2019 Jun;33(6):1659-1667.