Addition of pre transplant Rituximab to plasma exchange in FSGS children undergoing kidney transplantation
Marta Lidia Monteverde1, Marcos Paz1, Juan P. Ibanez1, Veronica Solernieu2, Luis Geovanni Cedeno1, Alicia B. Chaparro1.
1Nephrology, Hospital de Pediatria JP Garrahan, Ciudad Autónoma de Buenos Aires, Argentina; 2Pathology, Hospital de Pediatria JP Garrahan, Ciudad Autónoma de Buenos Aires, Argentina
Background: Recurrence of FSGS after kidney transplantation (KTx) is a significant risk factor for graft loss in children and adults. Data on the benefits of combined rituximab (RTX) and therapeutic plasma exchange (PE) in preventing unfavorable outcomes in this TX population are limited.
Aim: We compared the efficacy of the addition of pre-transplant RTX to PE for treatment of FSGS children vs a historical cohort treated with only PE
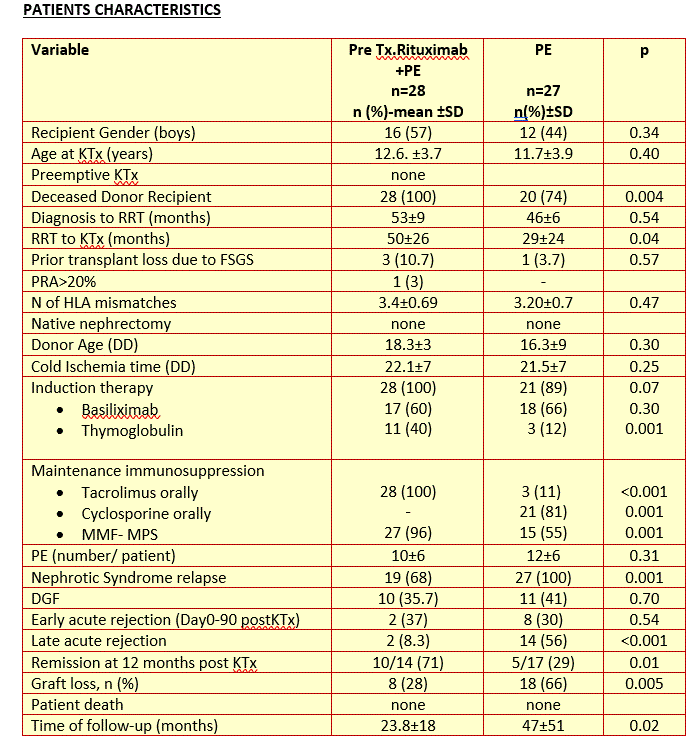
Patients and Methods: We included 28 patients treated between 2013-2019 with a combination of pretransplant RT and PE (RT + PE). For comparison we used a historical cohort treated between 1993-2013 with only PE (PE). Patients with confirmed or suspected FSGS mutations were excluded. Treatment protocol consisted of 1 dose of Rituximab (375mg / m2) given pre KTx. Patients with vascular access also received pre -Tx PE. Post KT children received a mean of 10 PE sessions (1=1.5 volemies, with 5% albumin replacement). As maintenance immunosuppression RT =PE received tacrolimus (100%) and PE group received cyclosporine (80%). In both groups, we analyzed recurrence of nephrotic syndrome, patient and graft survival, graft loss, remission at 12 months, early and late acute rejection (AR), and DGF.
Results: In the historic cohort, as PE was given because of relapse, relapse rate was 100%, and in those given RT+PE it was 68% (n=19). Patient survival at 1, 3 and 5 years was 100% in children who received RT+PE vs 100%, 85% and 85% in those who were on PE (p=0.2). Most frequent cause of death was bacterial sepsis (n=2). Graft survival at 1, 3 and 5 years was 81.3%, 67.1% and 53.7% in those with RT+ PE vs 63%, 43.5% and 43.5% in those on PE respectively (p=0.11). There were 41 graft losses; the most common cause of graft loss in both groups was relapse with or without rejection (n=18; 44%; 7 in RT+PE vs 11 in PE; p=0.18). Patients with RT + PE had lower rate of graft loss: 28% (8/28) vs 66% (18/27) in those with only PE (p=0.005); OR for graft loss: 0.2; CI95%: 0.05-0.72 for RT +PE. Remission rate at 12 months post KTx was 71% (10/14) in patients with RT + PE vs 29 % (5/17) in those only on PE (p=0.01). RT+PE patients were more likely to be on remission at 12-month post- KTx (OR:6; CI 95%: 1.02-37).DGF and early AR (Up to day 90 post KTx) rates were similar in both groups: 40% vs 35% (p=0.7) and 30% vs 37% (p=0.56). Late acute rejection was more prevalent among patients with only PE (56% vs 8.3%; p <0.001).
In this study pediatric FSGS patients given pre KTx RT+PE had lower risk of graft loss and were more likely to be on remission at 1-year post KTx compared to an historic cohort treated only with PE. DGF and early AR rates were similar in both groups. Late AR was more prevalent among children with only PE. Further prospective studies are needed to determine if preTX RT associated to PE is a better therapeutic option to only PE therapy in FSGS transplant children.
[1] Sami Alasfar. Transplantation . 2018 March ; 102(3): e115–e120. doi:10.1097/TP.0000000000002008.
[2] Lee Jin Koh.Pediatric Transplantation. 2019;23:e13469.DOI: 10.1111/petr.13469
There are no comments yet...