Intra-operative fluorescence angiography for renal graft perfusion assessment: An operative tool for post-transplant management
Giuseppe Ietto1, Caterina Franchi1, Valentina Iori1, Andrea Vigezzi1, Fabio Benedetti1, Elia Zani1, Federica Masci1, Cristiano Parise1, Domenico Iovino1, Mauro Oltolina1, Davide Brusa1, Sara Marzorati1, Linda Liepa1, Matteo Tozzi2, Giulio Carcano1.
1General, Emergency and Transplant Surgery Department, ASST-Settelaghi, Ospedale di Circolo e Fondazione Macchi, Varese, Italy; 2Vascular Surgery Department, ASST-Settelaghi, Ospedale di Circolo e Fondazione Macchi, Varese, Italy
Introduction: The introduction of extended criteria donor and the following larger use of marginal organs are responsible of an increasing number of “fragile” transplant with a raise in delayed graft function (DGF) rate. Accordingly, a tailored post-operative therapy has become critical. Our aim was to find intraoperative factors able to assess graft reperfusion in in order to early detect transplant at higher risk of DGF. To this end, we employed Indocyanine Green (ICG), a hydrosoluble fluorescent dye suitable and accurate for microvessels’ study, to perform an intraoperative fluorescent angiography and evaluate graft blood supply after reperfusion from a quantitative point of view.
Methods: We conducted a perspective clinical trial on 37 consecutive kidney transplants to explore accuracy, safety and feasibility of ICG angiography with fluorescence quantitative assessment. Pictures of the transplanted kidney are taken respectively 5, 15 and 45 minutes after reperfusion with a dedicated high definition fluorescent camera (Karl Storz Endoscopes®) after the injection of 3 doses of ICG properly diluted in saline solution (Verdye®). Images were then analysed with a specific open source software (ICY bioimage analysis®, Quantitative Image Analysis Unit, Institut Pasteur, Paris), which calculates the mean intensity value of fluorescence in a sample of graft parenchyma on the picture and its homogeneity. Data were Results: During one year from September 2018, we carried out 37 kidneys transplants. Considering the outcome at the time of discharge 27 (73%) transplanted patients experienced early graft function (EGF) and 9 (24.3%) patients underwent a delayed graft function (DGF). Only one graft (2.7%) never recovered its function (PNF – primary non-function). All transplanted kidneys that recovery immediately their function and therefore belonging to EGF group were endowed with a mean fluorescent intensity value egual or more than 49,953. In DGF group none kidney reached a fluorescence intensity over 55.648. In DGF group fluorescence intensity’s mean value was 96.930 ± 21, otherwise in EGF group was 37.718 ± 13; the analysis conducted performing Mann-Whitney U test has shown a statistically significant difference (p value < 0.0001). Quite the opposite the only kidney which never recovery has not overstepped the fluorescence intensity value of 25.220.
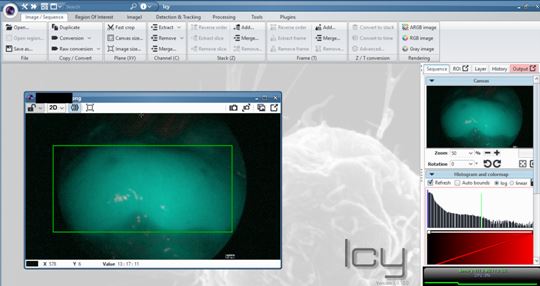
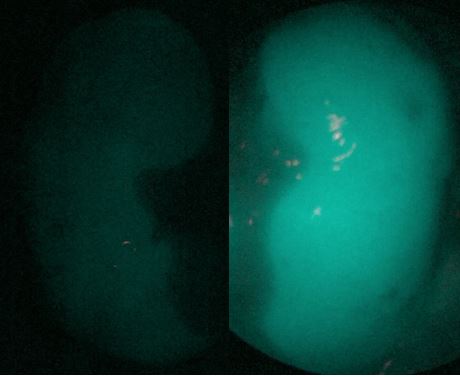
Conclusion: This method proved itself safe and risk-free, easily reproducible and without the need of different toolkit compared with those available in a modern operating theatre. The preliminary analysis shows a strong correlation between the data concerning perfusion so far obtained and the early outcome of the graft. Thus opening the way to further analysis aimed to a future better management of post-operative immunosuppressant and support therapy, based on a real time knowledge of graft microvasculature and then conditions of renal parenchyma.
[1] Metzger RA, Delmonico FL, Feng S, Port FK, Wynn JJ, Merion RM. Expanded criteria donors for kidney transplantation. Am J Transplant 2003;3 Suppl 4:114-25.
[2] Rother U, Gerken ALH, Karampinis I, et al. Dosing of indocyanine green for intraoperative laser fluorescence angiography in kidney transplantation. Microcirculation. 2017;24(8).
[3] Aslim EJ, Lee FJ, Gan VHL. The Utility of Intraoperative Near Infrared Fluorescence (NIR) Imaging with Indocyanine Green (ICG) for the Assessment of Kidney Allograft Perfusion. J Transplant 2018;2018:6703056.
There are no comments yet...