
A detailed analysis of the current status of intestinal transplantation in the Middle East
Hamed Nikoupour1, Peyman Arasteh1, Saman Nikeghbalian1.
1Shiraz Transplant Center, Abu-Ali Sina Hospital, Shiraz University of Medical Sciences, Shiraz, Iran (Islamic Republic of)
Introduction: Intestinal transplantations (IT) are among the most complex transplantations which are performed in few centers in the world. When patients develop intestinal failure, different treatment modalities including parenteral nutrition, autologous gastrointestinal tract reconstructive surgery and IT are considered. The Middle East is a region where reports on intestinal failures and IT are mainly lacking.
Materials and Methods: In the present review, we highlighted the status of IT in the Middle East and focused on existing reports from this region.
Results: From 2006 onward, the Shiraz Transplant Center has been the only center in Iran to perform this type of transplantation. So far, a total of 49 ITs have been performed in the center, among which 18 transplantations have been isolated ITs, 19 combined liver-intestine transplantations, 12 multi-visceral transplantations, and a total of 6 have been in the settings of modified multi-visceral transplantations. Two studies have been published in Turkey during the past ten years in which authors have reported on 9 patients who had ITs. All patient in Turkey had isolated IT. In the two reports authors found that the main etiology for IT in their center was Waardenburg syndrome (n = 4), malrotation (n = 2), trauma (n = 1), graft loss (n = 1) and megacystis microcolon intestinal hypoperistalsis (n = 1). Reports from Israel have been scarce. The first adult IT in Israel was performed in 2014 in the Beilinson Hospital, in Petah Tikva, Israel.
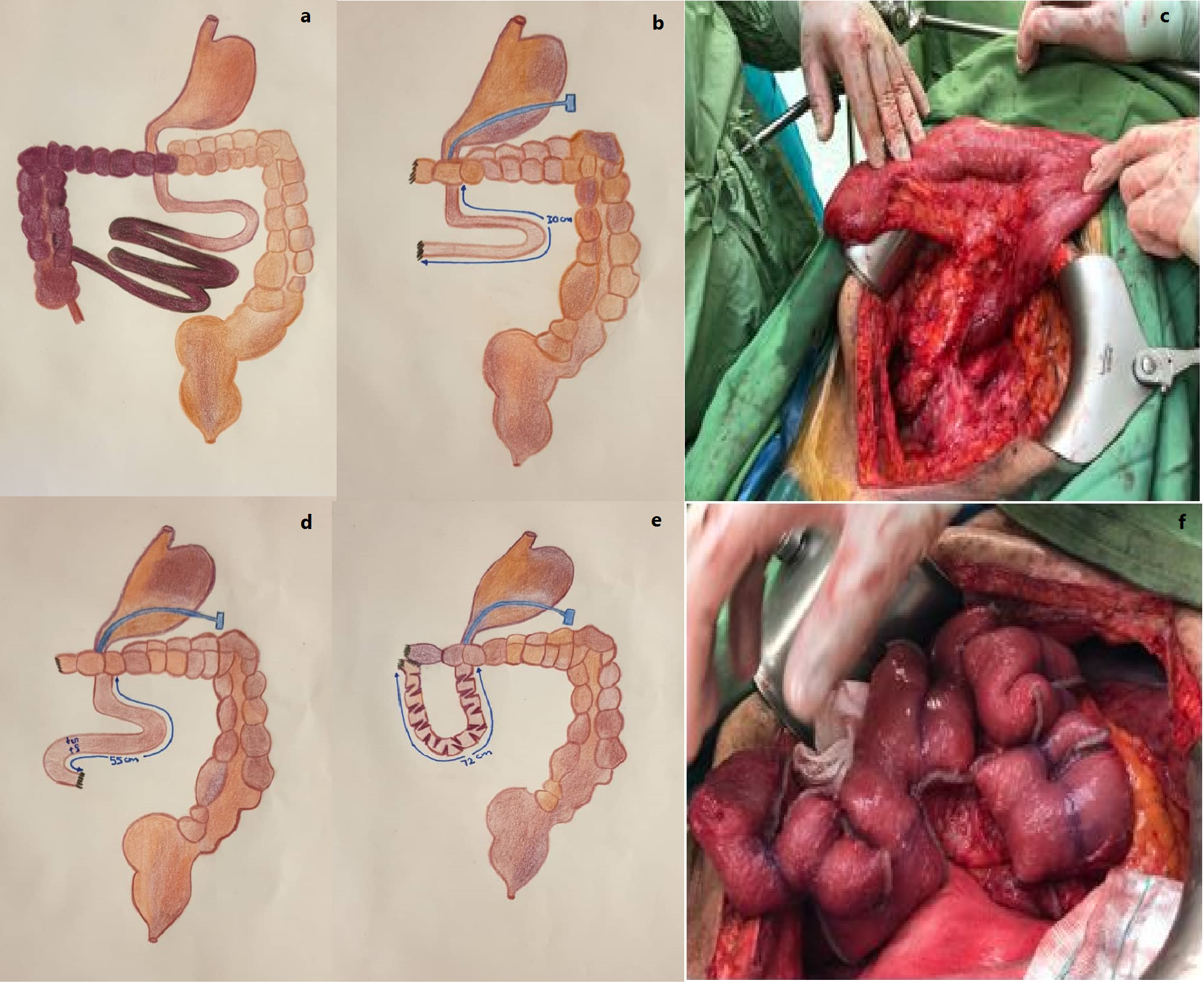
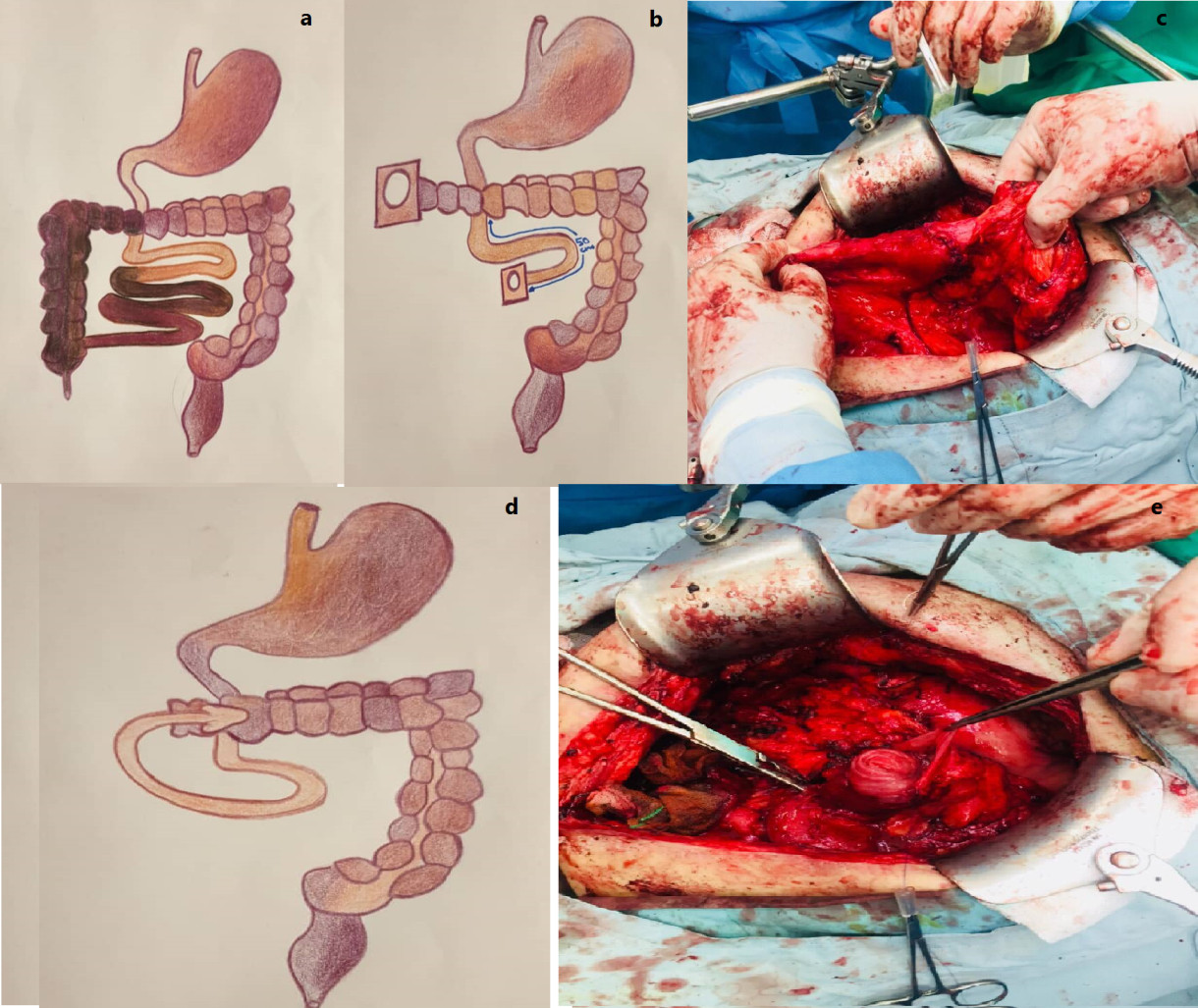
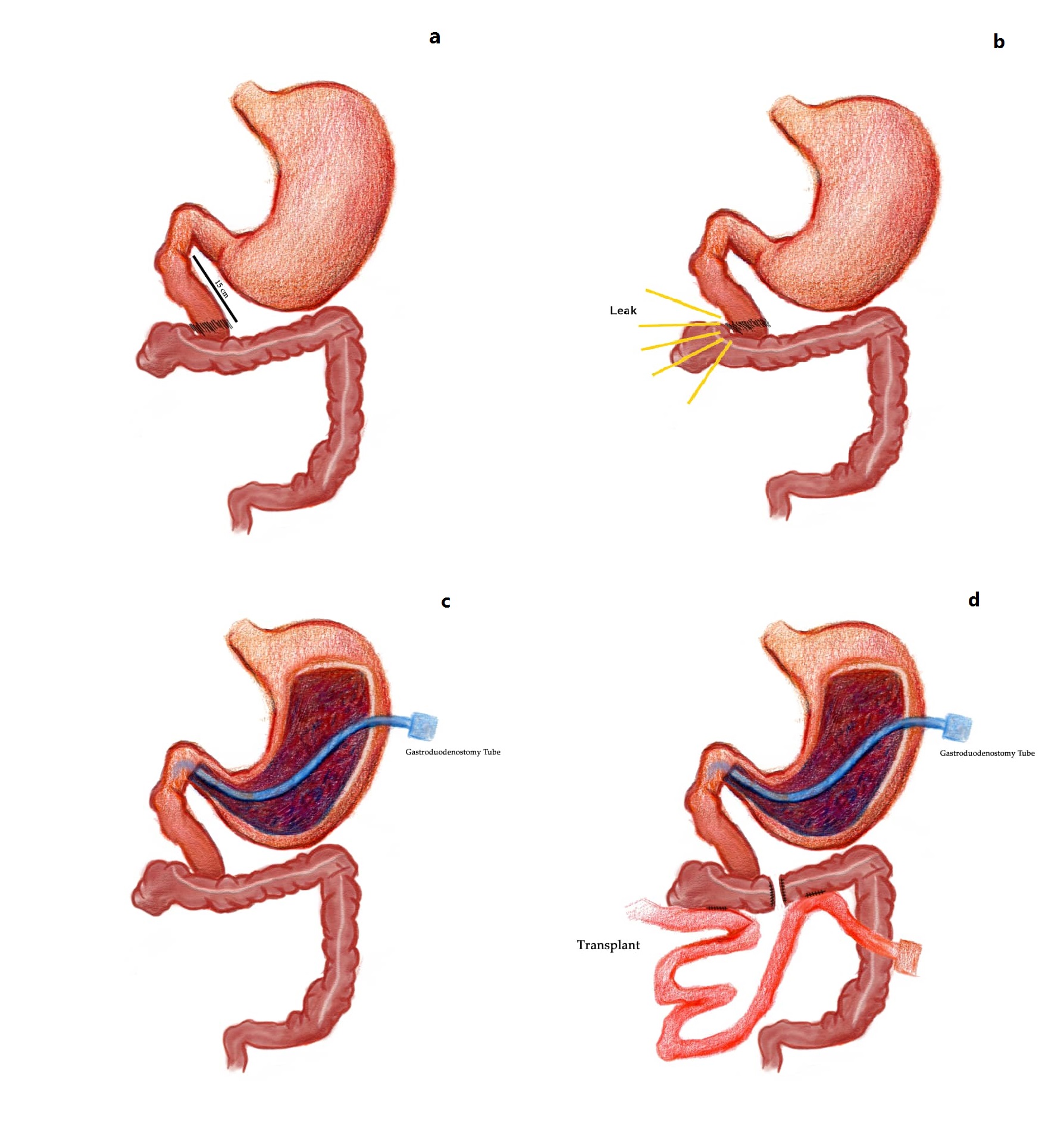
Discussion: Very few countries in the Middle East have the facilities for home parenteral nutrition and only two countries of Iran and Turkey perform ITs in the region. With advances in intestinal rehabilitation units and development of autologous gastrointestinal tract reconstructive surgery some centers have been able to reduce the number of patients in need of ITs.
Conclusion: An overview of the condition of ITs in the Middle East shows that the issue of intestinal failure and the treatment facilities still remain an unsolved problem. Although there exists a high need for IT, advances in reconstructive surgeries and the development of parenteral nutrition in this region, can significantly reduce the need for ITs among patients with intestinal failure.
[1] 1. Starzl TE, Todo S, Tzakis A, Alessiani M, Casavilla A, Abu-Elmagd K, et al. The many faces of multivisceral transplantation. Surgery, gynecology & obstetrics. 1991;172(5):335. 2. Starzl TE, Rowe MI, Todo S, Jaffe R, Tzakis A, Hoffman AL, et al. Transplantation of multiple abdominal viscera. Jama. 1989;261(10):1449-57. 3. Deltz E. Successful clinical small bowel transplantation: report of a case. Clin Transplantation. 1989;3:89-91. 4. Bharadwaj S, Tandon P, Gohel TD, Brown J, Steiger E, Kirby DF, et al. Current status of intestinal and multivisceral transplantation. Gastroenterol Rep (Oxf). 2017;5(1):20-8. 5. Elsabbagh AM, Hawksworth J, Khan KM, Kaufman SS, Yazigi NA, Kroemer A, et al. Long-term survival in visceral transplant recipients in the new era: A single-center experience. Am J Transplant. 2019;19(7):2077-91. 6. Pironi L, Steiger E, Brandt C, Joly F, Wanten G, Chambrier C, et al. Home parenteral nutrition provision modalities for chronic intestinal failure in adult patients: An international survey. Clin Nutr. 2019. 7. Abu-Elmagd KM, Kosmach-Park B, Costa G, Zenati M, Martin L, Koritsky DA, et al. Long-term survival, nutritional autonomy, and quality of life after intestinal and multivisceral transplantation. Ann Surg. 2012;256(3):494-508. 8. Grant D, Abu-Elmagd K, Mazariegos G, Vianna R, Langnas A, Mangus R, et al. Intestinal transplant registry report: global activity and trends. Am J Transplant. 2015;15(1):210-9. 9. Nikeghbalian S, Aliakbarian M, Kazemi K, Shamsaee far A, Salehipour M, Bahreini A, et al. Clinical experience in organ transplant from the Shiraz Transplant Center: 2011. Exp Clin Transplant. 2012;10(4):307-9. 10. Tugmen C, Baran M, Sert I, Anil AB, Kebapci E, Dogan SM, et al. Pediatric small bowel transplantation: A single-center experience from Turkey. Turk J Gastroenterol. 2016;27(5):428-32. 11. Bank TW. [Available from: https://data.worldbank.org/region/middle-east-and-north-africa. 12. [Available from: http://worldpopulationreview.com/continents/the-middle-east-population/. 13. Shaheen FA. Organ donation in the Middle East countries. Ethn Dis. 2009;19(1 Suppl 1):S1-16-7. 14. Gondolesi GE, Pattin F, Nikkoupur H. Management of intestinal failure in middle-income countries, for children and adults. Curr Opin Organ Transplant. 2018;23(2):212-8. 15. Al-Tawil ES, Almuhareb AM, Amin HM. Catheter-related blood stream infection in patients receiving long-term home parenteral nutrition: Tertiary care hospital experience in Saudi Arabia. Saudi J Gastroenterol. 2016;22(4):304-8. 16. Chermesh I, Mashiach T, Amit A, Haim N, Papier I, Efergan R, et al. Home parenteral nutrition (HTPN) for incurable patients with cancer with gastrointestinal obstruction: do the benefits outweigh the risks? Med Oncol. 2011;28(1):83-8. 17. Oz V, Theilla M, Singer P. Eating habits and quality of life of patients receiving home parenteral nutrition in Israel. Clin Nutr. 2008;27(1):95-9. 18. Theilla M, Kagan I, Chernov K, Cohen J, Kagan I, Singer P. Self-Evaluation of Quality of Life Among Patients Receiving Home Parenteral Nutrition: A Validation Study. JPEN J Parenter Enteral Nutr. 2018;42(3):516-21. 19. Grainger JT, Maeda Y, Donnelly SC, Vaizey CJ. Assessment and management of patients with intestinal failure: a multidisciplinary approach. Clin Exp Gastroenterol. 2018;11:233-41. 20. Pironi L, Corcos O, Forbes A, Holst M, Joly F, Jonkers C, et al. Intestinal failure in adults: Recommendations from the ESPEN expert groups. Clinical nutrition. 2018;37(6):1798-809. 21. Fusaro F, Morini F, Mutanen A, De Angelis P, Tambucci R, Capriati T, et al. Autologous Intestinal Reconstructive Surgery in the Management of Total Intestinal Aganglionosis. Journal of pediatric gastroenterology and nutrition. 2019;68(5):635-41. 22. Ramos-Gonzalez G, Kim HB, editors. Autologous intestinal reconstruction surgery. Seminars in pediatric surgery; 2018: Elsevier. 23. Celik N, Stanley K, Rudolph J, Al-Issa F, Kosmach B, Ashokkumar C, et al., editors. Improvements in intestine transplantation. Seminars in pediatric surgery; 2018: Elsevier. 24. Nobakht Haghighi A, Broumand B, Fazel I. Organ Transplantation in Iran before and after Istanbul Declaration, 2008. International journal of organ transplantation medicine. 2011;2(1):1-3. 25. Lappas BM, Patel D, Kumpf V, Adams DW, Seidner DL. Parenteral nutrition: indications, access, and complications. Gastroenterology Clinics. 2018;47(1):39-59. 26. Hurt RT, Steiger E. Early history of home parenteral nutrition: from hospital to home. Nutrition in Clinical Practice. 2018;33(5):598-613. 27. Marshall JK, Gadowsky SL, Childs A, Armstrong D. Economic analysis of home vs hospital-based parenteral nutrition in Ontario, Canada. JPEN J Parenter Enteral Nutr. 2005;29(4):266-9. 28. Cagan Appak Y, Baran M, Oztan MO, Karakoyun M, Turhan S, Tugmen C, et al. Assessment and outcome of pediatric intestinal pseudo-obstruction: A tertiary-care-center experience from Turkey. Turk J Gastroenterol. 2019;30(4):357-63. 29. Siegel-Itzkovich J. 1st intestinal transplant in Israel performed on 16-year-old girl April 22, 2008. 30. Efrati I. 'Breakthrough Procedure' Israeli Doctors Perform Country's First Intestine Transplant January 6, 2014. 31. Samuk I, Tekin A, Tryphonopoulos P, Pinto IG, Garcia J, Weppler D, et al. Abdominal transplantation for unresectable tumors in children: the zooming out principle. Pediatr Surg Int. 2016;32(4):337-46.
There are no comments yet...