
Building a self-sufficient liver transplant program in Mongolia
Ganzorig Banzragch1, Batsaikhan Batsuuri1, Bat-Ireedui Badarch1, Tamir Sainbuyan1, Sarnai Erdene2, Fidel Lopez-Verdugo3, Moustafa Moustafa4, Manuel I. Rodriguez-Davalos3, Sung-Gyu Lee5, Raymond R. Price4, Jade Nunez4, Sergelen Orgoi2.
1Liver Transplant, The First Central Hospital of Mongolia, Ulaanbaatar, Mongolia; 2Surgery, Mongolian National University of Medical Sciences, Ulaanbaatar, Mongolia; 3Transplant Services, Intermountain Medical Center, Salt Lake City, UT, United States; 4Center for Global Surgery, University of Utah, Salt Lake City, UT, United States; 5Liver Transplant, Asan Medical Center, Seoul, Korea
Introduction: The first liver transplant (LT) in Mongolia was performed in 2011. Since then, 93 more LTs have been performed. The aim of this study is to describe the establishment of a LT program with supervised learning and gradual program autonomy in a lower-middle income country (LMIC).
Materials and Methods: This is a retrospective study. Patients that received a LT between September 2011 and March 2020 were included. Demographic, transplant, and outcome data were collected.
In 2011, a partnership was established with an experienced liver transplant team from Korea to perform the first LT in Mongolia. During the first 4 years, all LTs were performed with the experienced team, with gradually increasing involvement of the Mongolian team.
Patients were classified as having been transplanted in the Initial Period (2011-2016), where most transplants were performed with the mentoring team, or the Current Period (2017-2020), performed mostly by the local team. Primary endpoints were patient and graft survival at 1-year. Safety outcomes included complication rates.
Results and Discussion: A total of 94 liver transplants were performed on 92 patients (88 adult and 4 pediatric) over the last 10 years. 30 patients received a LT during the initial period and 62 during the current period. LT activity has grown from 3 transplants performed in 2011 to 26 in 2019 (Fig 1).
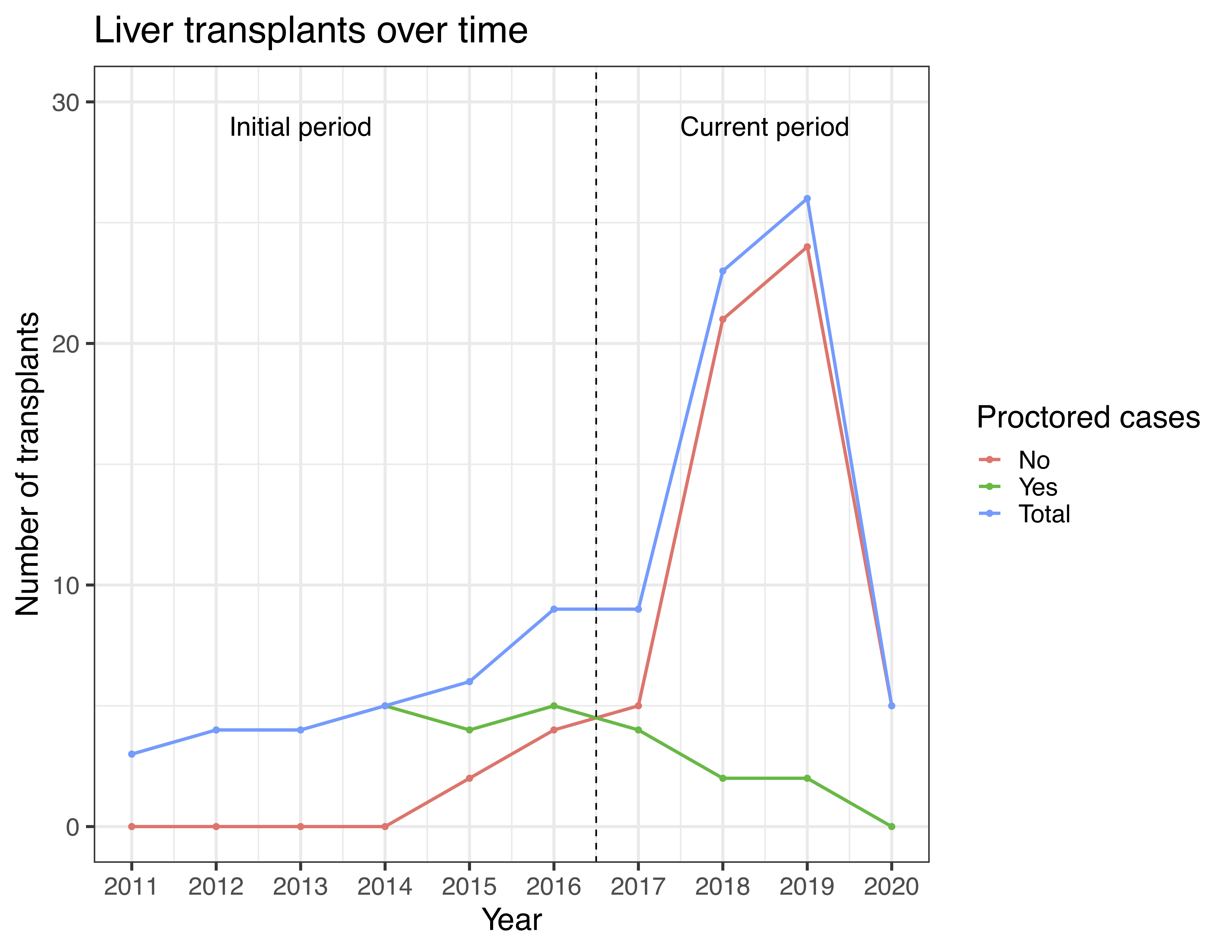
Since 2017, 87.3% of all LTs have been performed independently. 48.9% (45/92) of patients were female with a median age of 40.5 (IQR: 35-49) years old. The mean MELD at the time of transplant was 14.4±4.9 and the most common diagnosis was hepatitis B(HBV) (n=63) (Table 1).
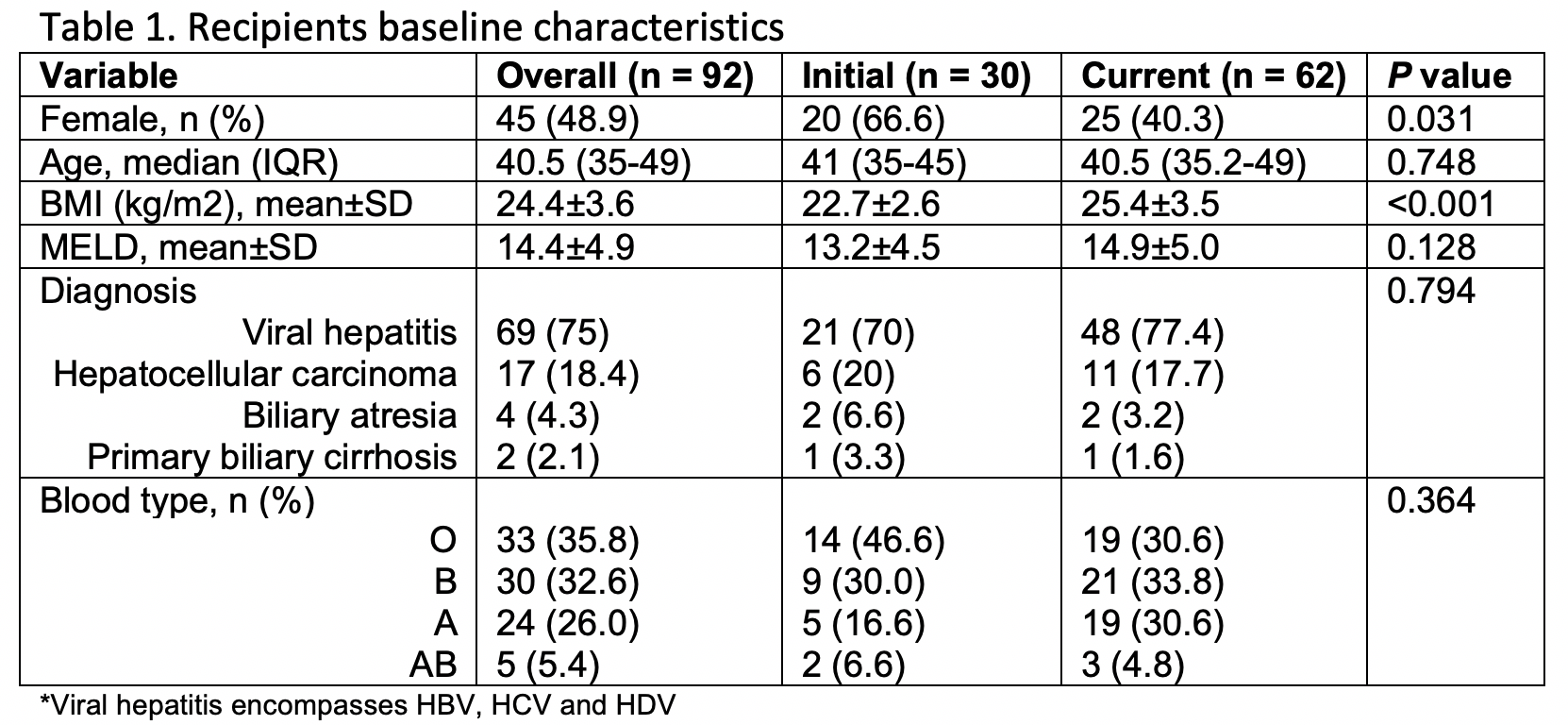
The majority of transplants were performed using right lobes from living donors (93.6%). All pediatric patients received a left lobe from living donors.
Nine (9.5%) patients had vascular complications, the most common being hepatic venous outflow obstruction (6.3%). Biliary complications were observed in 18 (19.1%) cases, most of which were biliary strictures (Table 2).
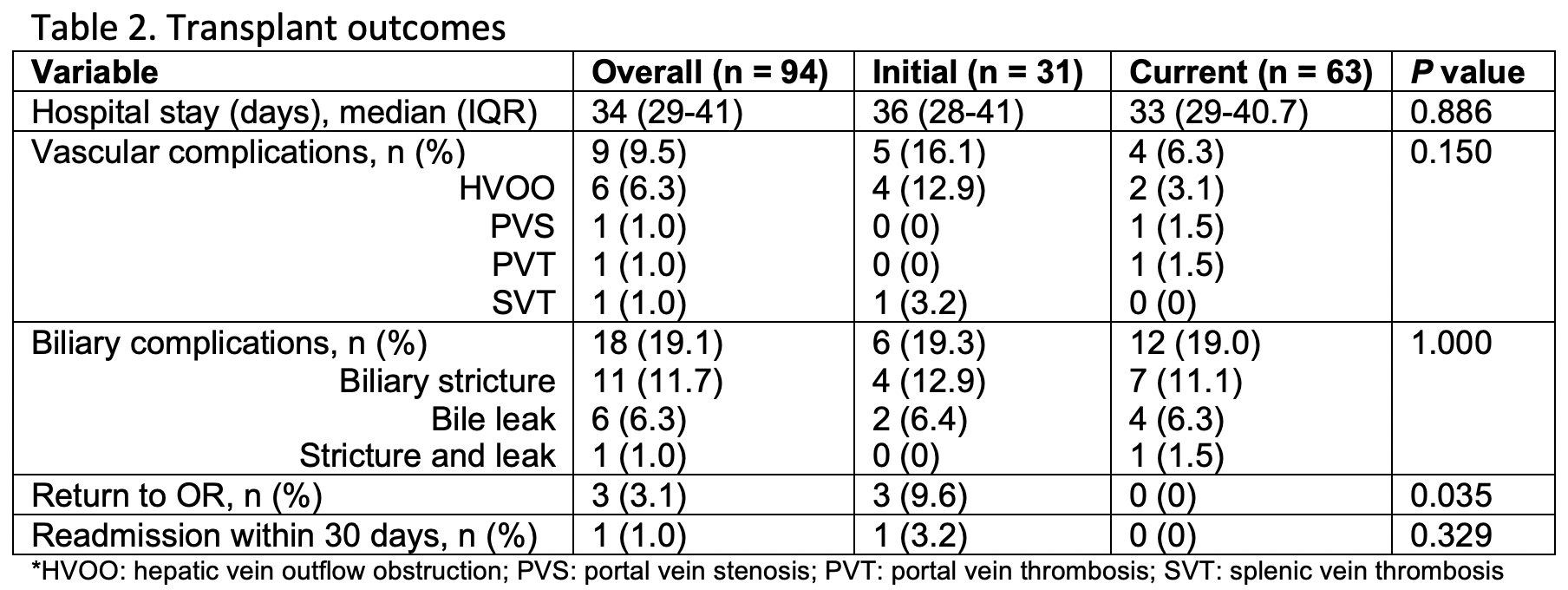
1-year survival was 93.9% (95% CI: 87.4-100), during the current period vs 93.3% (95% CI: 84.8-100) during the initial period (p = 0.6) (Fig 2A). Similarly, graft survival was 91.9% (95% CI: 84.5-99.9) for the current period and 90.3% (95% CI: 80.4-100; p = 0.75) for the initial period (Fig 2B).
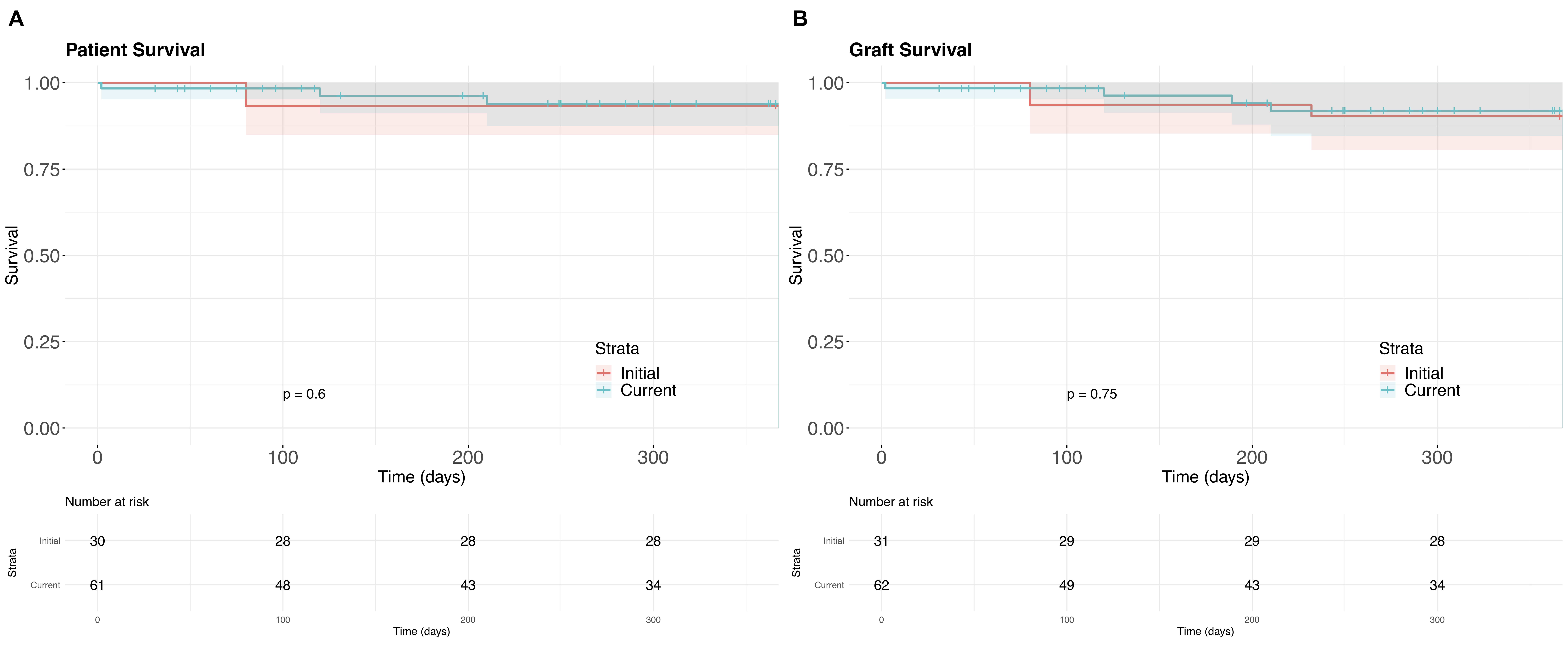
At 1 year, there were 5 deaths and 1 re-transplant.
Conclusion: The establishment of an independent LT program in a LMIC with outcomes similar to well established programs is feasible, and significantly increases access to life-saving procedures for patients with end-stage liver disease. LT volume increased five-fold after graduation to program autonomy. Further increases in capacity, however, are needed to meet the country’s demand. Greater utilization of deceased donors may be key to achieving this, in addition to strategies such as split liver transplants for children.
There are no comments yet...